AI predicts likelihood of disease
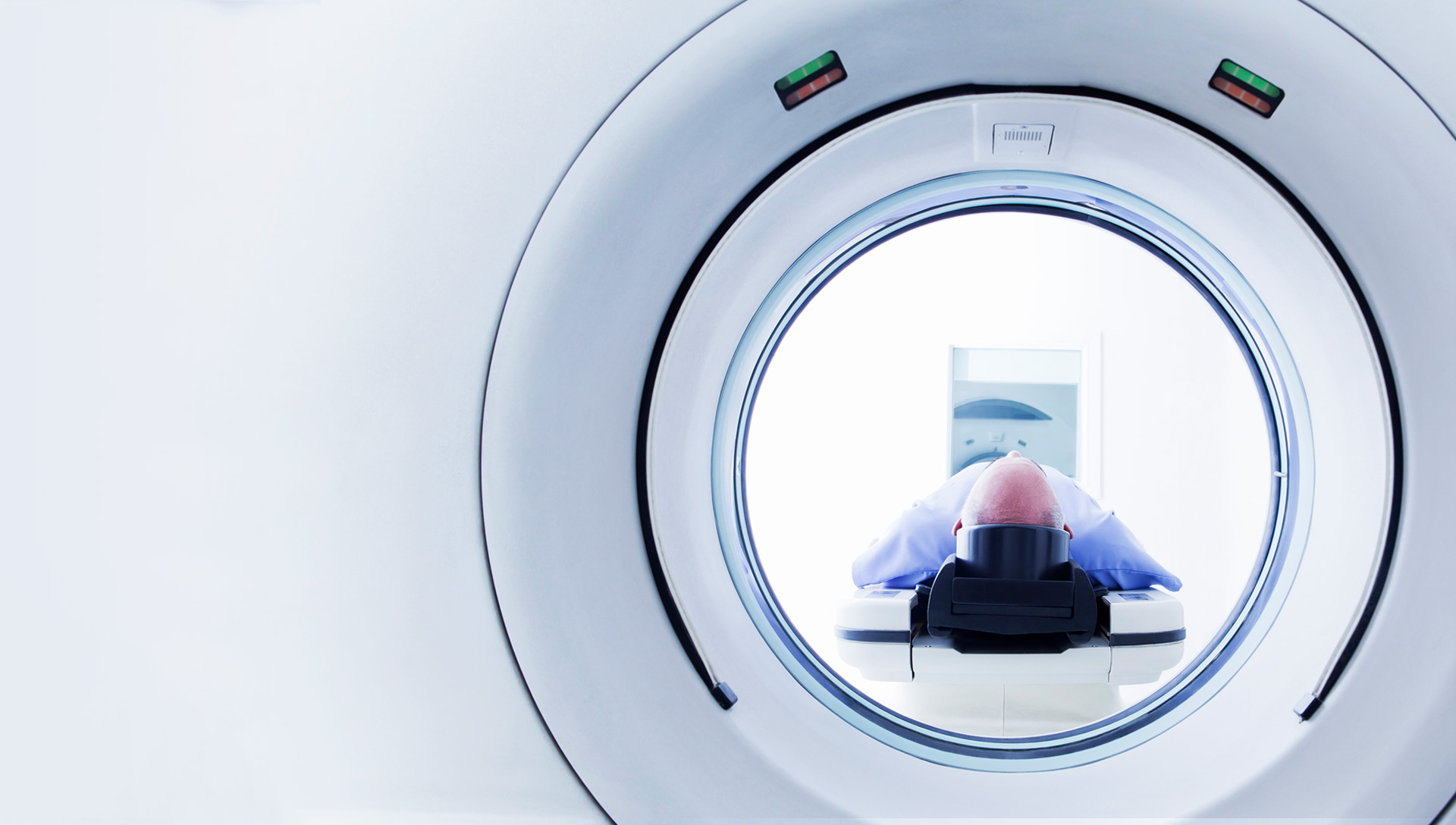
Operational efficiencies that improve healthcare delivery, while lowering readmissions, represent a welcome breakthrough, but even bigger benefits can be realized by disease prevention. Israel’s second largest health maintenance organization, Maccabi, is doing just that with its ColonFlag AI platform, which predicts 100 different conditions that can lead to colon cancer, stomach cancer, diabetes, sepsis, and organ dysfunction—all built using data available from medical records.
The platform employs machine learning to analyze millions of records, cross-referencing them with other medical knowledge and similar cases. A patient-specific prediction is produced, which peers six months, two years or five years into the future to crystallize the patient’s risk factors. A unique combination of algorithms and storage formats lets Maccabi work with large datasets to return accurate cognitive insights.8 For example, cognitive algorithms work with conventional algorithms that have been deconstructed and rewritten to optimize performance.
Medial EarlySign, founded in 2009, uses AI to improve patient health outcomes by isolating extraordinary clinical insights hidden in existing blood tests and EHR. In a study based on data from 645,000 prediabetes individuals, the technology discovered that by isolating less than 20 percent of the prediabetes population, its algorithm pinpointed 64 percent of individuals who became diabetic within a year.9
The FDA readies for change as digital medicine accelerates
The FDA is creating a new unit dedicated strictly to digital health in response to a growing workload that requires faster response than the organization is equipped to handle. Once again, AI is being assessed as a solution to the task of reviewing and garnering insight from huge volumes of text and reviewing applications to bring products to market.
Until now, it would take manufacturers years to get products ready for regulatory approval—and FDA reviewers could barely keep up. Now, as computer code is taking on more tasks (like spotting specious moles and quantifying blood flow), the workload is becoming overwhelming since software developers take months, not years, to ready a product for market. Through its digital health unit, the FDA is hiring software developers, AI experts, and cloud computing experts in order to prepare the agency to regulate a future in which health care is increasingly mediated by machines.
AI and robotics
In San Francisco, Dr. Cory Kidd (CEO and founder, Catalina Health) has built an AI-powered robot dedicated to motivating its owners into positive behavioral changes. Kidd’s invention, named Mabu, is a desktop companion with a touchpad on her belly. As a personal healthcare companion, Mabu helps patients manage chronic diseases. With her wide green eyes and yellow skin, she is often compared to one of the personified feelings in the Pixar movie Inside Out. But, as we live longer and put more stress on an already overburdened healthcare system, AI and robotics may provide a much-needed contribution.
Says Mabu user Martha Singleton, “She’s here to mainly remind us of our medications. She’s a robot, but in a way, you feel that she actually cares when she does things that a friend would do, like calling my doctor.” As society moves towards an alarming scenario where there are not enough people to deliver healthcare services, robotics and AI could provide a viable solution to fill the gap by monitoring your health, sending encrypted data to your doctor, and reading your emotions. Robots won’t replace the healthcare worker—rather, they’ll augment the capacity for healthcare workers to handle larger numbers of patients.10